Suffer from hayfever? A solution may be at hand...
A new clinical trial from joint research with Imperial College and King’s College could bring an end to the summer sneezing
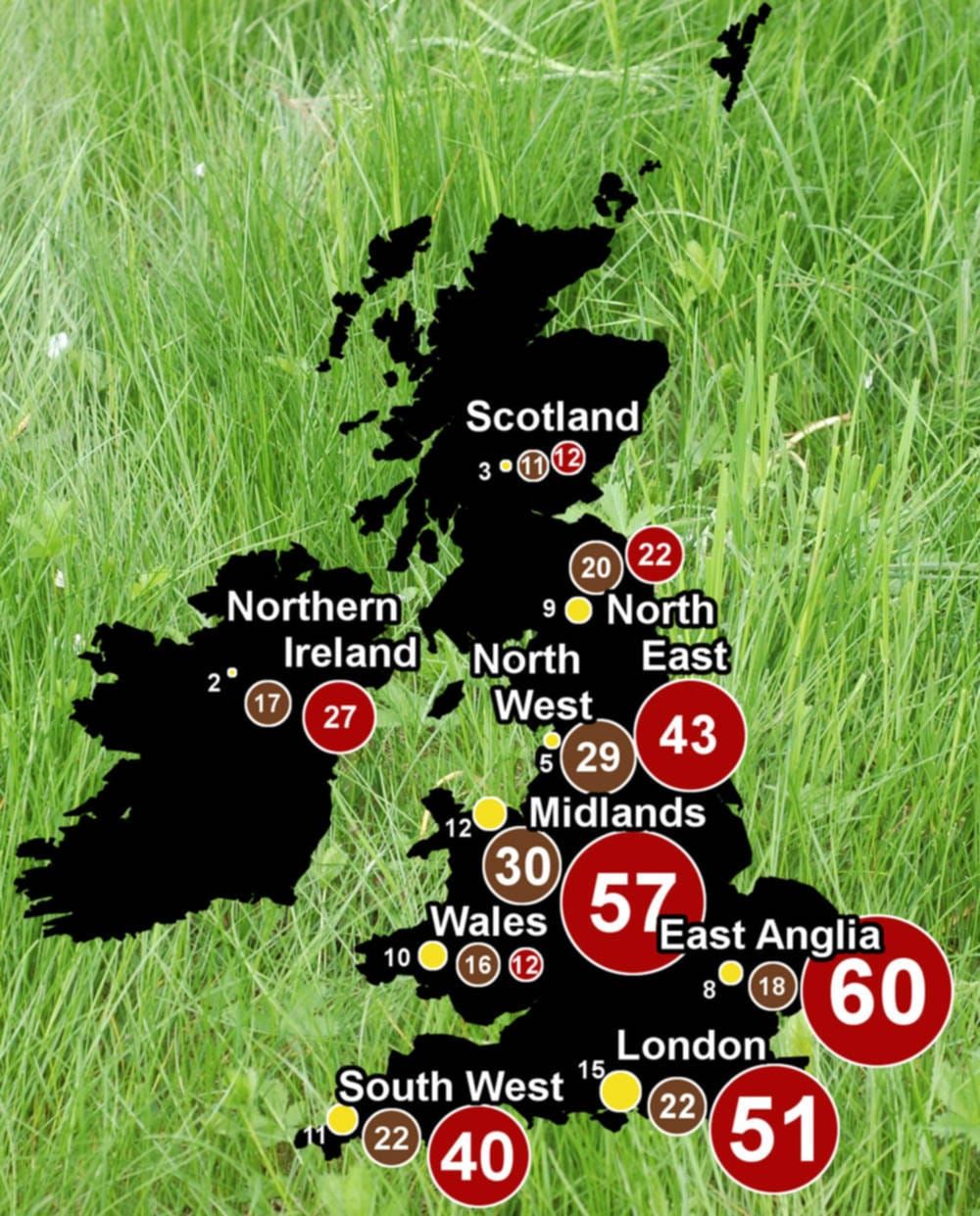
What is hayfever?
A little history...
First scientifically described in 1819 by John Bostock, hay fever, also known as allergic rhinitis, is an allergic reaction to small particles in the air that most commonly causes nasal inflammation but may also result in watery eyes and itching throat. These symptoms are the result of the airborne allergens triggering the production of histamine, which produces inflammation. While most people experience only mild effects the condition can cause severe disruption in people lives and may exacerbate the symptoms of asthma.
Allergy or something else?
Despite the condition’s name, hay very rarely produces an allergic reaction. Sufferers instead find themselves hypersensitive to wind distributed pollen, most commonly that of grass, which is responsible for some 90% of cases, but also that of certain trees (such as birch) and other plants.
While pollen levels are generally highest in late spring and early summer, different weeds flower through the entire period from early spring to autumn; hay fever symptoms may also be caused by dust, pet hair and fungal spores — meaning that some people experience the condition year round.
95% of hayfever sufferers are allergic to grass pollen
In rare cases ‘cross-reactivity’ may occur — with hay fever sufferers experiencing an allergic reaction to certain foods, such as apples, which contain similar proteins to those found in pollen grains.
Some one fifth of the population experience hay fever, and while it can affect anybody it is most common amongst those with a family history of allergies. The condition usually first manifests in the early teens and reduces in severity in the sufferer’s 20s — in up to 20% of cases, all symptoms permanently dissapear in the end.
Natural Remedies
For all the hippies out there, you will be sorry to hear that alternative cures are somewhat lacking when it comes to significant remedial properties. Complementary Alternative Medicine, also lovingly referred to as CAMs, consist of yoga, homeopathy and herbal medicines, and up to 70% of sufferers have been known to give these a go in there times of need. Meanwhile, some literature suggests that acupuncture may relieve some symptoms.
Acupuncture is an age old Chinese remedy that is based on the principle that humans have energy
Sufferers say their productivity is reduced by 63%
“flows” throughout the body, and that the balances of these such “flows” can be disturbed, resulting in pain. Naturally the correction of these flows is done via the insertion of needles into exact points on the body surface, and some people truly swear by it.
However, if you are a sceptical scientist like all Imperial students should be, consider with caution the legitimacy of this, as published trials are sketchy in both the methodology and the results they present.
But if you still can’t face putting money into GSK’s ever expanding pocket, consider “herbal medicines”. Despite modern medicine having primarily plant-based derivatives anyway, many Earth-lovers consider it acceptable to categorisetheir own, poorly standardised medicine niche as “herbal” to rid them of the guilt of using them.
If this applies to you, at least aim to use plants such as butterbur (a girly little daisy), which was proven by one trial to be similar in effect as fexofenadine, a commonly used anti-histamine.
However, as with all herbal medicines, you run the risk of suffering from adverse side effects and potentially high toxicity exposure, alongside pharmacological interactions with other drugs that may be taken that are still not understood.
What is PollenLITE?

PollenLITE is a new type of vaccine aiming to prevent hay fever symptoms triggered during grass pollen season. Instead of treating the symptoms, like the over-the-counter anti-histamines found in your local pharmacist, pollenLITE prevents these symptoms in the first place by “turning off” the allergic reaction.
The potential for a vaccine like pollenLITE was first hinted at in a study published in 2011, where researchers at Imperial discovered that long-term tolerance to grass pollen is accompanied by special “blocking” antibodies remaining in the body.
Earlier this year, a study by the same group found that repeatedly exposing people to low doses of
78% of hayfever sufferers feel it detrements their quality of life
grass pollen beneath the skin can cause these antibodies to appear, and so create a long-term tolerance to grass pollen.
The evidence from these studies triggered the clinical trial for pollenLITE – a potential hay fever vaccine that uses smaller doses and shallower injections compared to previous versions.
PollenLITE is currently in the recruiting phase for volunteers, with an advertising campaign including Tube adverts, for trial injections starting in early 2013.
Current remedies
Antihistamines
Antihistamines are a group of over the counter drugs currently used to treat hay fever and other allergic reactions. As the name suggests, they work by counteracting the effects of histamine. They do this by acting as antagonists on the H1 histamine receptor. Histamine is an inflammatory mediator released by mast cells in response to immunoglobulin E activation (caused by an allergen such as pollen). Its release in the nasal mucosa causes inflammation, leading to the symptoms of hay fever: nasal congestion, runny nose, itchiness, and sneezing.
There are two broad classes of antihistamines: first generation and second generation. First generation antihistamines are “sedating”. They cause drowsiness because they can cross the blood-brain barrier and act on the central nervous system as well as the periphery. Examples of these
54% of sufferers feel less attractive using peak periods
include promethazine, chlorphenamine and clemastine. Second generation antihistamines are larger and less lipophilic molecules. This means they cross the blood-brain barrier less readily, and are therefore less likely to cause drowsiness. For this reason, they are usually recommended over the first generation drugs. Examples of second generation antihistamines include cetirizine, loratadine and fexofenadine.
Corticosteroids
Corticosteroids are a form of steroid treatment, and this come with the usual warnings that steroids usually have: mood swings, weight gain, and acne. However they have the benefit of being an incredibly effective form of treatment. They also have the benefit of being a usable form of treatment for pregnant women, and those who do not respond to antihistamines.
There is also a difference in the method of administration, with most corticosteroids being in the form of eye drops or nasal sprays. This makes them incredibly useful if a hay fever sufferer has severe eye irritation, though tablets are also available. It is also possible to obtain antihistamines in eyedrop form.
Similar treatments
Approaches that involve training the immune system to prevent hay fever from manifesting are called immunotherapy, of which there are two kinds.
The first of these is called SLIT, or sublingual immunotherapy, involves placing a pill under the tongue, which dissolves. This pill contains a small amount of pollen.
A clinical trial, in associationwith Royal Brompton and Harefield NHS Trust, was conducted last year to investigate the long-term effectiveness of two much-praised pills, Alutard SQ and Grazax. This includes a campaign to attract volunteers, including the advert seen above in Felix last year.
This research was led by Professor Stephen Durham, from the faculty of Medicine at Imperial College London, who has large amounts of experience in this field. The aim was to find whether the pill form was as, or more, effective than injections, which would remove the need for the inconvenient method of administration for people who use this form of treatment.
The second type is called SIT, or systemic injection immunotherapy, where the pollen is injected into the skin.
PollenLITE is an example of this kind. Such an approach is not new, with vaccines having existed for a long time, however the difference between this and previous approaches is a less intrusive way of administration, thanks to the shallower injection needed.
Both kinds of immunotherapy require multiple administrations to build up the necessary level of immunity, with it possibly requiring up to a year until the symptoms of hay fever are no longer felt. With this in mind, less intrusive methods are always desired.








